Infertility is a complex and often emotionally challenging condition that affects millions of people worldwide. While many are familiar with common causes such as hormonal imbalances, ovulation disorders, or male factor infertility, there are lesser-known conditions that can have an equally profound impact. One such condition is Asherman syndrome.
Asherman syndrome is a disorder in which scar tissue forms inside the uterus, leading to partial or complete blockage of the uterine cavity. This seemingly localized problem can have far-reaching consequences, particularly for women trying to conceive. Because the uterus plays a central role in implantation and pregnancy development, any disruption to its structure can significantly reduce fertility.
Despite its importance, Asherman syndrome is often underdiagnosed or misunderstood. Many women may go through multiple unsuccessful attempts at conception before the condition is identified. In some cases, symptoms are subtle or even absent, making awareness even more critical.
This article provides an extensive exploration of Asherman syndrome, covering its causes, mechanisms, symptoms, diagnosis, treatment, and long-term outlook. It is written to be accessible to the general reader while also serving as a useful study resource.
Understanding the Normal Uterus and Endometrium
To fully grasp how Asherman syndrome affects fertility, it is important to first understand how a healthy uterus functions.
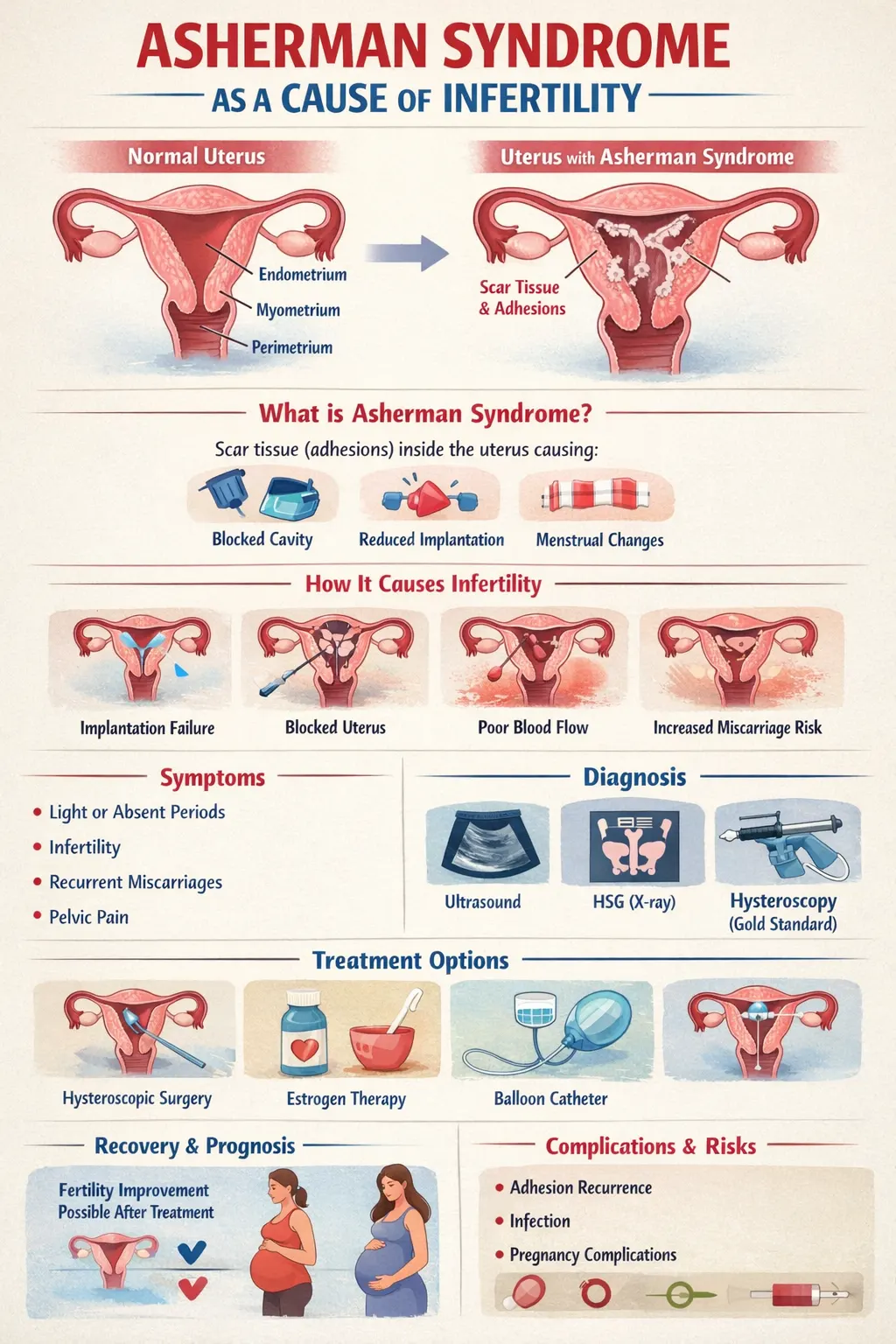
Structure of the Uterus
The uterus is a hollow, muscular organ located in the pelvis. It consists of three main layers:
-
Endometrium (inner lining)
-
Responsible for menstrual cycles
-
Site of embryo implantation
-
-
Myometrium (muscular layer)
-
Contracts during menstruation and childbirth
-
-
Perimetrium (outer layer)
-
Protective covering
-
The Role of the Endometrium
The endometrium is especially important for fertility. Each month, under hormonal influence, it:
-
Thickens in preparation for pregnancy
-
Becomes rich in blood vessels
-
Creates a receptive environment for embryo implantation
If fertilization does not occur, the lining sheds during menstruation.
In Asherman syndrome, this delicate lining is damaged and replaced with scar tissue, disrupting the entire reproductive process.
What Is Asherman Syndrome?
Asherman syndrome is defined by the presence of intrauterine adhesions—bands of fibrous scar tissue that form inside the uterine cavity.
Key Characteristics
-
Adhesions may be thin or dense
-
They can partially or completely block the uterus
-
The normal uterine cavity may become distorted or obliterated
These adhesions essentially “stick” the walls of the uterus together, reducing the space available for normal endometrial function.
Why It Matters
The condition directly impacts:
-
Menstrual function
-
Implantation of embryos
-
Maintenance of pregnancy
Even small adhesions can interfere with fertility, while severe cases may completely prevent conception.
Causes of Asherman Syndrome
The most common cause of Asherman syndrome is trauma to the uterine lining. This trauma often occurs during medical procedures.
1. Dilation and Curettage (D&C)
This is the leading cause.
D&C involves scraping or suctioning the uterine lining and is commonly performed after:
-
Miscarriage
-
Abortion
-
Retained placenta
Repeated procedures significantly increase risk.
2. Postpartum Complications
After childbirth, the uterus is particularly vulnerable. Procedures to remove retained tissue or control bleeding can damage the endometrium.
3. Cesarean Section
While generally safe, complications such as infection or excessive tissue damage can lead to adhesion formation.
4. Uterine Infections
Severe infections can destroy the endometrial lining.
Examples include:
-
Endometritis
-
Tuberculosis affecting the uterus (rare but serious)
5. Surgical Procedures
Other uterine surgeries may contribute:
-
Fibroid removal
-
Polyp removal
-
Septum correction
How Asherman Syndrome Causes Infertility
The connection between Asherman syndrome and infertility is both structural and functional.
1. Loss of Implantation Surface
Scar tissue replaces healthy endometrium, reducing the area available for embryo attachment.
2. Impaired Blood Supply
Adhesions often lack proper blood vessels, meaning:
-
Nutrient delivery is compromised
-
Embryo survival becomes unlikely
3. Mechanical Obstruction
Adhesions can physically block:
-
Sperm from reaching the egg
-
Embryo from implanting
4. Hormonal Disruption
Even if hormones are normal, the uterus may not respond appropriately due to damaged tissue.
5. Increased Miscarriage Risk
Even if implantation occurs, the abnormal environment can lead to pregnancy loss.
Symptoms of Asherman Syndrome
Symptoms vary widely depending on severity.
Menstrual Changes
-
Light periods (hypomenorrhea)
-
Absent periods (amenorrhea)
-
Irregular cycles
Fertility Issues
-
Difficulty conceiving
-
Recurrent miscarriages
Pain
-
Pelvic pain
-
Cyclical pain without bleeding
Silent Cases
Some women experience no obvious symptoms but still face infertility.
Risk Factors
Certain conditions increase the likelihood of developing Asherman syndrome.
Major Risk Factors
-
Multiple D&C procedures
-
Postpartum uterine interventions
-
Uterine infections
Additional Risks
-
Aggressive surgical techniques
-
Poor healing response
-
Lack of follow-up care
Diagnosis of Asherman Syndrome
Early diagnosis is critical for effective treatment.
Medical History
Doctors evaluate:
-
Previous pregnancies
-
Surgeries
-
Menstrual changes
Imaging Tests
Ultrasound
-
May suggest abnormalities
-
Limited accuracy
Hysterosalpingography (HSG)
-
Uses contrast dye
-
Shows uterine shape
Gold Standard: hysteroscopy
This procedure allows direct visualization of the uterus and is the most reliable diagnostic method.
Classification of Severity
Mild
-
Thin adhesions
-
Minimal cavity distortion
Moderate
-
More extensive scarring
-
Partial blockage
Severe
-
Dense adhesions
-
Near or complete closure of uterus
Treatment Options
Treatment aims to restore the uterine cavity and improve fertility.
1. Surgical Treatment
Hysteroscopic Adhesiolysis
-
Adhesions are cut and removed
-
Uterine cavity is restored
2. Hormonal Therapy
Example: estrogen
-
Promotes endometrial healing
-
Encourages regrowth
3. Mechanical Devices
Used to prevent re-adhesion:
-
Balloon catheters
-
Intrauterine devices
Post-Treatment Care
Proper care after surgery is essential.
Follow-Up Procedures
-
Repeat hysteroscopy
-
Imaging tests
Monitoring
-
Menstrual cycle normalization
-
Endometrial thickness
Fertility Outcomes After Treatment
Success Rates
-
Mild cases: high success
-
Severe cases: lower but possible
Pregnancy Outcomes
-
Many women conceive naturally
-
Some may require assisted reproduction
Assisted Reproductive Technologies
If natural conception is not successful, options include:
-
IVF (in vitro fertilization)
-
Hormonal stimulation
These methods may bypass some barriers but still depend on uterine health.
Complications
Surgical Risks
-
Infection
-
Uterine perforation
Recurrence
Adhesions may return, especially in severe cases.
Pregnancy Risks After Treatment
Women with a history of Asherman syndrome may face:
-
Placenta previa
-
Placenta accreta
-
Preterm birth
Careful monitoring is required.
Prevention Strategies
Medical Practices
-
Avoid unnecessary D&C
-
Use gentle techniques
Patient Awareness
-
Seek care after abnormal periods
-
Follow up after procedures
Psychological Impact
Infertility can deeply affect mental health.
Emotional Effects
-
Anxiety
-
Depression
-
Relationship strain
Coping Methods
-
Counseling
-
Support groups
-
Education
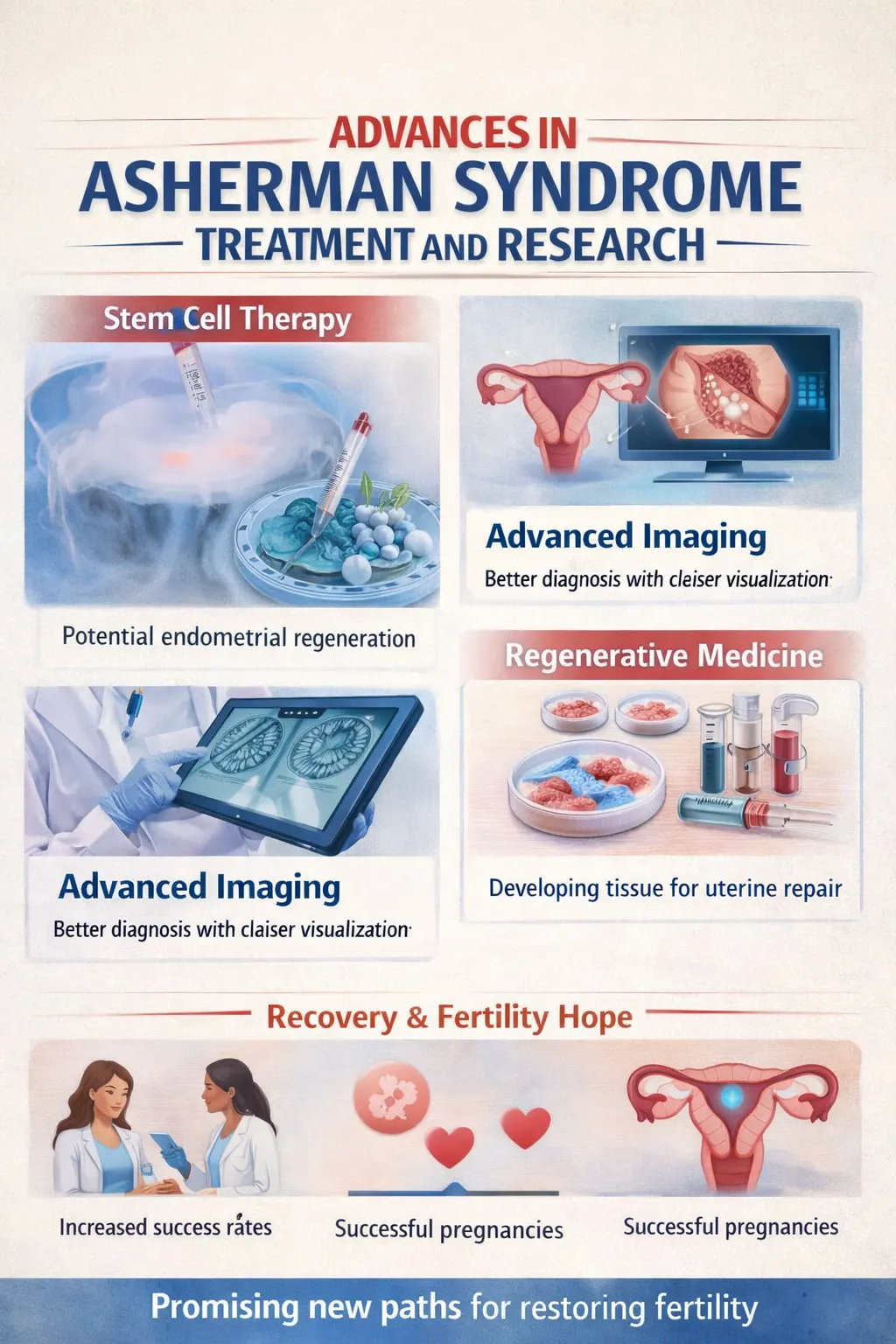
Advances in Research
New treatments are emerging.
Promising Developments
-
Stem cell therapy
-
Regenerative medicine
-
Improved surgical tools
Lifestyle Considerations
While Asherman syndrome is structural, overall health still matters.
Helpful Practices
-
Balanced diet
-
Stress management
-
Regular medical checkups
When to Seek Medical Help
Consult a doctor if you experience:
-
Changes in menstruation
-
Difficulty conceiving
-
History of uterine procedures
Conclusion
Asherman syndrome is a complex but treatable condition that can significantly impact fertility. While it may be overlooked in many cases, increased awareness and modern medical techniques have greatly improved diagnosis and treatment outcomes.
Understanding the condition empowers individuals to seek timely medical care, ask informed questions, and explore appropriate treatment options. With proper management, many women affected by Asherman syndrome can achieve successful pregnancies and restore reproductive health.